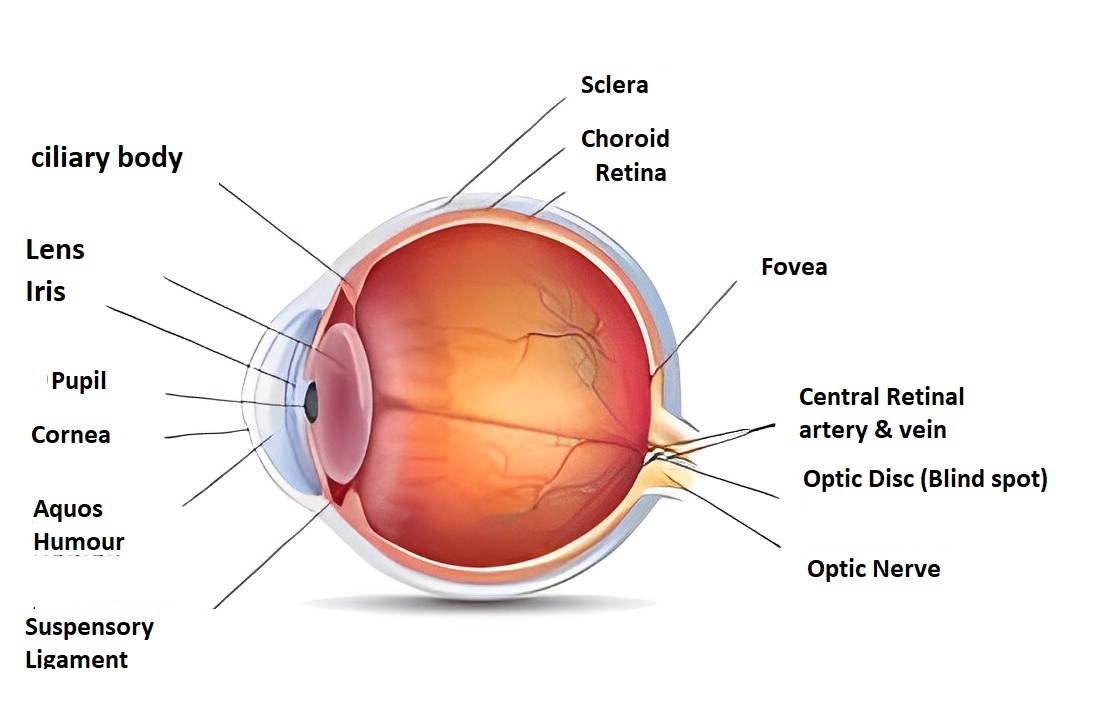
Descemet’s membrane is an essential component of the cornea, which is the clear, dome-shaped tissue that covers the front of the eye. It is a thin, translucent layer of tissue that acts as a barrier between the stroma of the cornea and the eye’s endothelial layer.
The Descemet’s membrane is critical for preserving the shape and clarity of the cornea, and its malfunction can result in a variety of corneal diseases. The anatomy, function, and diseases of Descemet’s membrane will be discussed in this blog article.
Descemet’s Membrane Anatomy
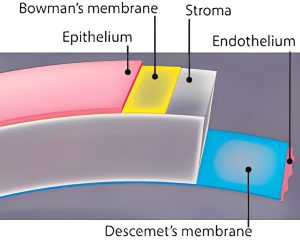
The Descemet’s membrane is an acellular, thin layer of the cornea positioned between the stroma and the endothelial layer. It is made up of collagen fibers and glycosaminoglycans and is thicker towards the edges of the cornea than in the center. The membrane is around 10-15 microns thick and is thinnest in the center of the cornea.
Function
The Descemet membrane is essential for the structural integrity of the cornea. It provides a smooth surface for endothelial cells to rest on and aids in the preservation of the cornea’s structure and thickness. It also serves as a barrier, keeping endothelial cells from migrating into the stroma and preserving the clarity of the cornea.
Disorders
Descemet’s membrane is linked to a number of corneal diseases. Fuchs’ Endothelial Dystrophy is the most prevalent of these illnesses, a progressive disease that damages the endothelial cells of the cornea and causes Descemet’s membrane thickening and guttae development.
Another condition that causes Descemet’s membrane alterations and the production of aberrant endothelial cells is posterior polymorphous corneal dystrophy. Corneal hydrops is an uncommon condition in which Descemet’s membrane ruptures, allowing fluid into the cornea and causing sudden corneal edema and visual loss.
(Read More About Degloved Face: Definition, Signs and Symptoms, Treatment and Preventions)
Signs and Symptoms of Descemet’s Membrane Disorders:
- Corneal edema (swelling)
- Blurred vision
- Eye pain or discomfort
- Sensitivity to light
- Halos or glare around lights
- Eye redness
Diagnosis:
- Ophthalmic examination with a slit-lamp microscope to examine the cornea
- Pachymetry, a test that measures corneal thickness
- Endothelial cell count to assess the number of cells lining the back of the cornea
- Corneal topography to evaluate the shape and curvature of the cornea
- Specular microscopy, a type of imaging test that allows visualization of the endothelial cells
Management:
- Treatment of underlying conditions, such as diabetes or inflammation
- Use of hypertonic saline drops or ointments to reduce corneal swelling
- Use of contact lenses to improve vision
- Corneal transplant surgery if the condition is severe and vision is significantly affected
Treatment:
- Treatment depends on the severity of the condition
- Conservative management options are usually the first line of treatment
- Surgery may be necessary in severe cases, including partial or full corneal transplant
- If you experience any of the signs or symptoms mentioned above, it is important to see an ophthalmologist for a proper diagnosis and treatment plan.
Conclusion:
Descemet’s membrane is an important component of the cornea that contributes to its structure and transparency. The membrane is connected with several illnesses, and their diagnosis and management necessitate a complete understanding of its anatomy and function. Early detection and treatment of these illnesses are critical to preventing vision loss and preserving the health of the cornea.
FAQs
Q: What is the thickness of Descemet’s membrane?
A: The thickness of Descemet’s membrane ranges from 8 to 12 micrometers in humans.
Q: What happens if Descemet’s membrane is damaged?
A: If Descemet’s membrane is damaged, it can lead to corneal edema (swelling), which can cause blurred vision and discomfort. In some cases, a partial or full-thickness transplant of the cornea may be necessary to repair the damage.
Q: Can Descemet’s membrane be regenerated?
A: Descemet’s membrane has limited regenerative capacity. In some cases, the endothelial cells that line the back surface of the cornea can regenerate and produce a new layer of Descemet’s membrane.
Q: What conditions can affect Descemet’s membrane?
A: Descemet’s membrane can be affected by various conditions, including Fuchs’ endothelial corneal dystrophy, posterior polymorphous corneal dystrophy, and iridocorneal endothelial syndrome.
Q: How is Descemet’s membrane studied?
A: Descemet’s membrane can be studied using various imaging techniques, such as confocal microscopy, anterior segment optical coherence tomography, and specular microscopy.
References:
Ljubimov, A. V. (2016). Descemet’s membrane and corneal endothelium: structure and function. Experimental eye research, 154, 14-23.
McLaughlin, C. N., & Anderson, N. G. (2021). Descemet’s Membrane. In StatPearls [Internet]. StatPearls Publishing.
Sorkin, N., Einan-Lifshitz, A., & Mimouni, M. (2021). Imaging of Descemet’s membrane. Survey of ophthalmology, 66(6), 897-912.
You May Also Like
- Premenstrual Syndrome (PMS) Explained: Powerful Relief Strategies for 2026
- Magnetic Seizure Therapy (MST): A Breakthrough in Psychiatric Treatment in 2025
- AIIMS New Delhi, NIMHANS Bengaluru, JIPMER Puducherry: No Leaves for Healthcare Workers Amid Tensions
- Narcissistic Personality Disorder in 2025: Unveiling the Hidden Struggles and Empowering Recovery
- Conquering Rubral Tremor: Unveiling Effective Treatments in 2025